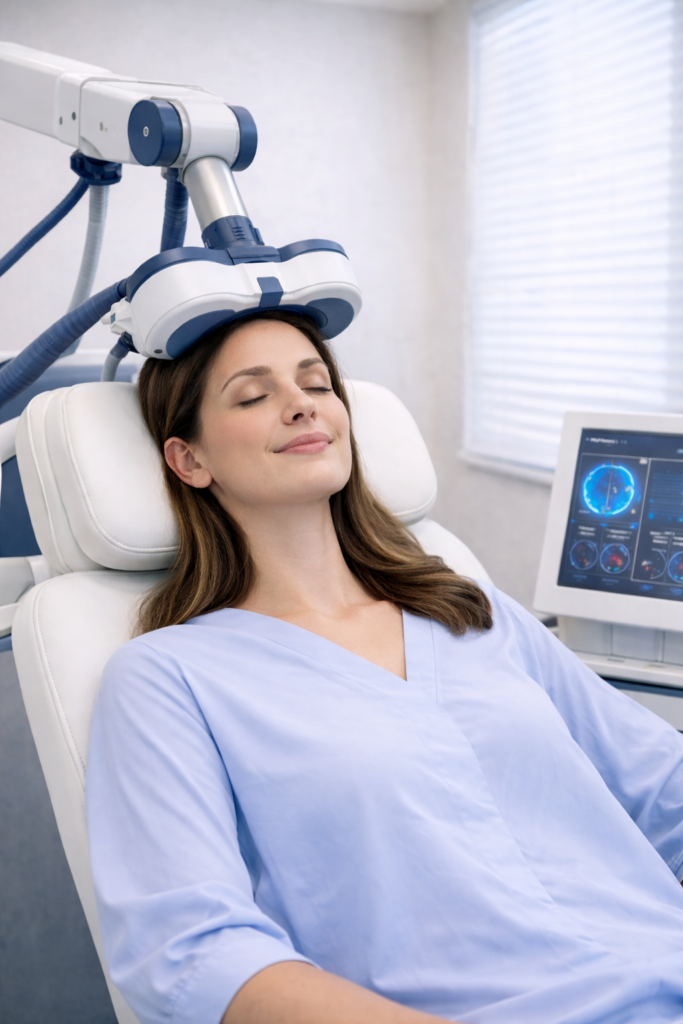
Introduction to TMS in Miami
Transcranial Magnetic Stimulation TMS in Miami may be an option for adults whose depressive symptoms continue to affect daily life or who want to discuss additional treatment approaches with a qualified provider. As interest in noninvasive mental health treatments continues to grow, many patients are asking whether TMS should be part of their treatment conversation.
At Miami Mental Health & Wellness, TMS is approached as part of a broader mental health care discussion rather than as a one-size-fits-all answer. That distinction matters. Depression can affect sleep, focus, energy, motivation, and emotional balance in different ways from one person to another. Because of that, treatment decisions should be based on a careful review of symptoms, treatment history, and current mental health needs rather than on general information alone.
What TMS Is
Transcranial Magnetic Stimulation, commonly known as TMS, is a noninvasive treatment that uses magnetic pulses to stimulate specific areas of the brain involved in mood regulation. It does not involve surgery, and it does not require general anesthesia. Sessions are typically performed while the patient is awake in an outpatient setting, which makes it a structured option that can be discussed within a larger mental health treatment plan.
Why More Patients Are Asking About TMS
Patients often begin exploring TMS when depressive symptoms remain difficult to manage or when previous treatment approaches have not led to enough improvement. Others simply want to understand whether there are additional options available beyond what they have already tried. TMS is often part of that conversation because it offers a different type of treatment approach, but it still requires individualized evaluation before moving forward.
How Transcranial Magnetic Stimulation TMS in Miami Works
Brain Stimulation and Mood Regulation
TMS works by delivering repeated magnetic pulses to targeted brain regions associated with mood regulation. These areas are involved in how the brain processes emotions, motivation, and certain patterns linked to depression. The purpose of treatment is not to offer a quick fix, but to explore whether stimulating these brain regions may be clinically appropriate as part of a patient’s care plan.
Why TMS Is Considered Noninvasive
One reason many patients ask about Transcranial Magnetic Stimulation TMS in Miami is because it is noninvasive. There is no surgery, no implanted device, and no need for general anesthesia. Since the treatment is typically provided while the patient is awake in an outpatient office setting, it can fit into a broader care routine more easily than some people expect. Still, convenience should never replace proper evaluation. At Miami Mental Health & Wellness, the focus is on whether TMS makes sense for the individual patient, not simply whether it is available.
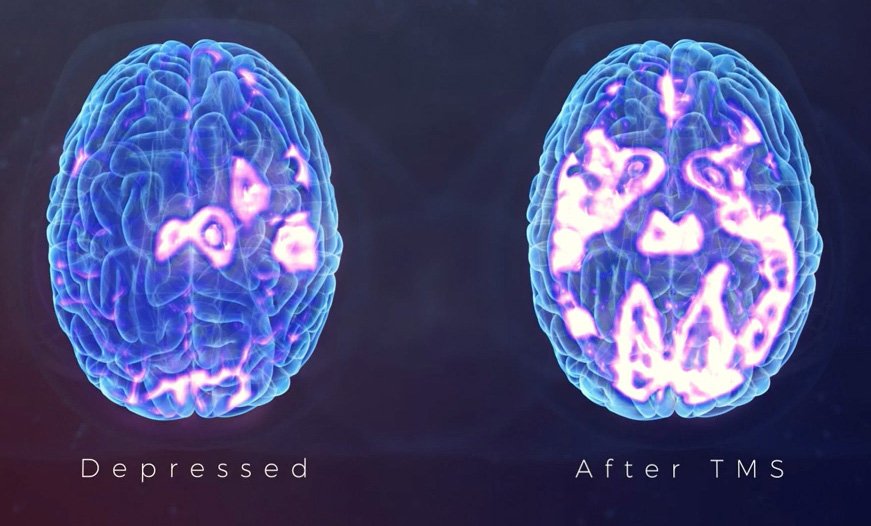
When TMS May Be Considered
Ongoing Depressive Symptoms
TMS may be considered when depressive symptoms continue to interfere with daily functioning. Some patients report persistent low mood, reduced motivation, poor concentration, or difficulty maintaining routines at work, school, or home. When symptoms remain present over time, it may be reasonable to review whether additional treatment options should be discussed with a provider.
When Previous Treatment Has Not Helped Enough
In some cases, patients begin asking about TMS because previous treatment approaches have not provided enough improvement. That does not automatically mean TMS is the next step, but it may mean the treatment conversation should expand. A provider may review what has already been tried, how symptoms have changed over time, and what the patient’s current goals are before deciding whether TMS should be explored further.
Why a Clinical Evaluation Matters
Reading about TMS online can be helpful, but self-diagnosis should not guide treatment decisions. A professional evaluation helps clarify whether symptoms are primarily related to depression or whether other mental health factors may also need attention. At Miami Mental Health & Wellness, the clinical team evaluates each patient individually to determine whether TMS should be part of the discussion based on symptoms, treatment history, and overall mental health needs.

What a TMS Session May Feel Like
What Happens During Treatment
TMS is typically performed in an outpatient office setting. During the session, the patient remains awake while the device is positioned for treatment. Because sessions are structured and repeated over time, treatment is usually discussed as a course of care rather than a single appointment. This helps frame TMS within a realistic and clinically grounded treatment plan.
Common Patient Experience During a Session
Some people describe the sensation of TMS as tapping on the scalp during the procedure. Experiences can vary, which is why patients benefit from having the chance to ask questions before treatment begins. Since TMS does not require sedation, many patients are able to continue normal daily activities after their appointment. Even so, expectations should be based on a provider’s guidance and not on assumptions from general articles or social media content.
Who May Be a Candidate for TMS
Factors Reviewed by a Provider
A patient may be a candidate for TMS when depressive symptoms are persistent, treatment history suggests a need to review other options, and a provider determines that this approach may be clinically appropriate. Candidacy is not based only on symptoms. It may also depend on medical history, current mental health needs, previous care, and other clinical factors that affect suitability.
Why Personalized Evaluation Matters
At Miami Mental Health & Wellness, candidacy for TMS is determined through a personalized evaluation process. That matters because mental health treatment should be aligned with the patient’s actual needs, not based on a general checklist. Individualized review helps ensure that treatment planning remains clinically grounded and focused on what is most appropriate for that person’s situation.
TMS as Part of a Broader Mental Health Plan
TMS Alongside Therapy or Medication Management
TMS is not always treated as a standalone answer. In many cases, it may be considered as one part of a broader mental health plan that also includes psychiatric evaluation, medication management, therapy, or ongoing follow up. This is important because depression often overlaps with other concerns such as stress tolerance, emotional regulation, concentration difficulties, and changes in daily functioning.
The Importance of Ongoing Follow Up
Mental health care often works best when treatment is reviewed over time rather than approached as a single decision. Ongoing follow up gives patients the opportunity to discuss progress, ask questions, and make informed treatment decisions as their needs change. At Miami Mental Health & Wellness, TMS is considered within the context of continuing care rather than in isolation from the rest of the patient’s symptoms and goals.
Why Local Access in Miami Matters
Continuity of Care
Local access matters because mental health treatment often requires continuity. When patients can receive evaluation, treatment planning, and follow up in one setting, the process may feel more manageable and more consistent over time. That can make it easier to stay engaged in care and maintain communication with the clinical team.
Receiving Treatment in One Clinical Setting
For adults in Miami and South Florida, working with a local practice such as Miami Mental Health & Wellness can help simplify the treatment process. Patients can discuss symptoms, review treatment options, and ask questions about TMS in a familiar clinical environment. That level of continuity supports more informed decision-making and a more personalized care experience.
Frequently Asked Questions
What is Transcranial Magnetic Stimulation TMS?
Transcranial Magnetic Stimulation TMS is a noninvasive treatment that uses magnetic pulses to stimulate specific brain areas involved in mood regulation.
Does TMS require surgery or anesthesia?
No. TMS is noninvasive and does not require surgery or general anesthesia.
What may a TMS session feel like?
Some patients describe the treatment as a tapping sensation on the scalp during the procedure. Experiences may vary from person to person.
Who decides whether I am a candidate for TMS?
A qualified provider should determine candidacy after reviewing symptoms, treatment history, overall mental health needs, medical history, and other relevant clinical factors.
Can TMS be part of a larger treatment plan?
Yes. TMS may be considered alongside other mental health services such as psychiatric evaluation, therapy, medication management, and ongoing follow up.
Does Miami Mental Health & Wellness offer TMS evaluations?
Yes. At Miami Mental Health & Wellness, the clinical team evaluates whether TMS should be part of the treatment discussion based on the patient’s symptoms, history, and overall needs.
Conclusion
Transcranial Magnetic Stimulation TMS in Miami may be worth discussing when depressive symptoms remain difficult to manage or when other treatment approaches have not provided enough improvement. While TMS is not the right fit for everyone, it can be an important option to explore as part of a personalized treatment discussion.
At Miami Mental Health & Wellness, TMS is approached as one possible component of a broader mental health treatment plan, with individualized evaluation guiding each step of the process. For adults in Miami who want to better understand whether this treatment may be appropriate for their needs, a professional clinical review is the right place to begin.